One of the most common problems experienced by denture-wearers is denture stomatitis. Of the 20% of people in the UK who wear dentures, ⅔ of them have this infection. There are different reasons why it develops.
Some people are at a higher risk of developing it than others, and it is slightly more common in females than males. The problem is that not many people are aware that they even have it. So, understanding it is important to get early treatment and prevent it from worsening.
What Is Denture Stomatitis?
Denture stomatitis is an infection of the mouth, most commonly caused by Candida albicans (yeast). It is believed that trauma to the soft tissue of the oral cavity results in this infection. However, the susceptibility of the host to this infection also plays a role in this.
Normally, the oral cavity contains an innocuous amount of this yeast. However, it becomes problematic when its percentage increases to 60-100%. It should be noted that Candida albicans isn’t the only fungus associated with this infection. It can also attract others like Candida glabrata (which uses Candida albicans to establish itself) and Candida auris.
This kind of infection most commonly occurs in the upper jaw, more specifically, the palate. It is unlikely for you to pass it on to someone else, but it is possible if the other person is susceptible to it. In order to determine whether or not you have this, your doctor will perform a physical exam and take an oral swab to send it for testing.
What Are the Three Types of Denture Stomatitis?
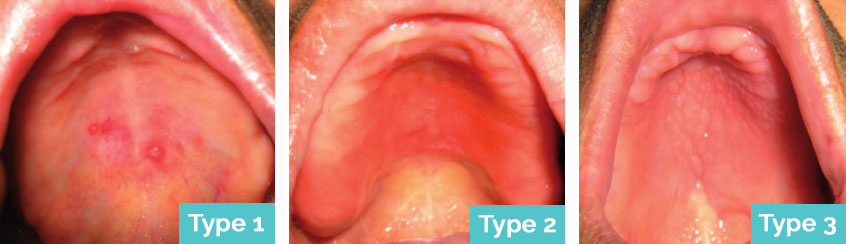
Three classifications of denture stomatitis were presented in 1962 by Newton. These are as follows:
- Newton Type 1 – The mildest form, characterised by localised inflammation.
- Newton Type 2 – The moderate form, characterised by generalised inflammation. It can affect a part of the area where the dentures are worn or all of it.
- Newton Type 3 – This is the most severe form, characterised by inflammatory papillary hyperplasia (a benign lesion in the oral cavity). It requires surgical removal.
What Are the Symptoms of Denture Stomatitis?
When it’s mild, patients don’t experience any symptoms of this infection. However, in its more severe forms, it can cause the following:
- Pain/discomfort
- Impaired taste
- Difficulty swallowing
- Itchiness or burning sensation
- Swelling
- Redness and irritation
- Oral thrush
- Plaque on dentures
- Cracked corners of the mouth
Denture stomatitis can also result in aspiration pneumonia when harmful microorganisms are inhaled into the lungs. It can be fatal.
What Causes Denture Stomatitis?
Following are the potential risk factors and causes of denture stomatitis:
Poor Denture Hygiene
It is one of the main reasons why denture stomatitis can develop. Improper cleaning of the dentures and poor oral hygiene can result in the growth of the fungi responsible for this infection.
You can further exacerbate this problem by consuming foods that are high in sugar. These can make the saliva more acidic, which makes it easier for C. albicans to stick better and grow even more.
Continuous Use of Dentures
Another significant risk factor for denture stomatitis is wearing them for a very long time or not removing them. Doctors usually recommend taking them off before sleeping so that the saliva can wash over the gums and clean them.
In addition, it allows your gums to rest. Wearing it all the time can result in trauma to the tissue, which makes it more vulnerable to infection.
Dry Mouth (Xerostomia)
The decreased production of saliva (which can result from wearing dentures) can cause the proliferation of yeast in the mouth. Without saliva to cleanse the surface of the dentures and oral cavity, the yeast is likely to stay put.
Another problem with dry mouth is that it can cause problems with the retention of the dentures, which can cause trauma to the soft tissues.
Worn Surface of Dentures & Acrylic Resin
Having dentures for a very long time can result in wear and tear. Eventually, the surface may become rough, with small fissures and cracks. These small pockets give the yeast a more permanent lodging.
Using abrasive toothpaste and brushes can speed up the process. In addition, it is seen that dentures made of acrylic are rougher with cracks in them. This makes it easier for them to thrive.
Smoking
Denture-wearers are advised not to smoke because it can result in denture stomatitis. There are different ways in which smoking makes it easier for yeast to thrive in the mouth. It does the following:
- Suppresses the immune system
- Changes in the oral microbiome
- Decreases the production of saliva
- Reduces the pH of saliva
According to a study published in BMC Oral Health, denture stomatitis is twice as common in smokers than in non-smokers.
Other Causes
Although not as significant, the following can also cause denture stomatitis:
- Diabetes
- HIV
- Hematologic disorders
- Immune disorder
- Nutritional deficiencies (Vitamin A, D, folate, etc.)
- Antibiotics and steroids
People who have any of these problems are more likely to develop this infection.
How To Treat Denture Stomatitis?
The following treatments may be suggested by your doctor if the abnormal presence of yeast is confirmed:
Antifungals
Medicines like nystatin, fluconazole, and miconazole are commonly used for the treatment of oral yeast infections. Clotrimazole is also used, but because its troches contain sugar, it’s not as suitable for patients with diabetes. Antifungals are available in the form of lozenges, gels, rinses, and suspensions.
Usually, a topical treatment is prescribed. That’s because lozenges and suspension can make a person feel nauseous or vomit. It can also cause an upset stomach. Taking the tablets for a long-time is also not the first course of action because of the side effects associated with it.
This treatment can also be followed by a dental cleaning/scale and polish session. Furthermore, the denture is also checked, whether it needs to be made or relined.
Laser & Surgery
According to the European Association of Oral Medicine (EAOM), if the patient has Newton-type 1 or 2 denture stomatitis, the oral surgeon can use a low energy laser to treat the inflammation.
However, in the case of the lesion, surgical removal is needed as it can affect the proper fitting of the denture. The surgeon can use a scalpel, high-frequency electrical currents (electrosurgery) or extreme cold (cryosurgery) to remove the lesion.
How To Prevent Denture Stomatitis?
It is possible to prevent denture stomatitis if you do the following:
Maintain Good Denture & Dental Hygiene
You should ensure that you have good dental hygiene in order to prevent denture stomatitis, as it is one of the biggest reasons why it develops. You should continue brushing your gums, tongue and palate using a soft-bristled brush twice a day. In addition, you need to use an antimicrobial mouthwash.
Moreover, you should make sure to clean the denture itself using a non-abrasive toothbrush. When not in use, soak it in a solution and do not wash it in boiling water. Your doctor may also recommend using chlorhexidine to rinse the dentures. Some research also shows that using “natural” cleansers like apple cider vinegar, citric acid, and baking soda can prevent the yeast from sticking to the dentures. However, discuss this with your doctor first.
Get Dental Implants
Instead of wearing removable dentures, you can consider getting them implant-supported. That’s because as the jawbone shrinks after tooth loss, it can affect the fitting of the dentures.
Trauma to the underlying tissue can result from a bad fit, which is a precursor to denture stomatitis. You will get enough stimulation from implants to keep your bone from shrinking and changing shape. Therefore, it can help prevent this infection.
Make Lifestyle Changes
One way to prevent denture stomatitis is to make some lifestyle changes. That includes not smoking and eating foods that aren’t rich in carbohydrates. In addition, you need to make sure that you’re not wearing your dentures for a very long time. Take them off at night or whenever possible.
Conclusion
Denture stomatitis is usually a result of an infection caused by some species of yeast. Despite the fact that some people are more prone to it due to certain risk factors, it is thought to be caused by trauma to the oral tissue. This can only make it more vulnerable to attack by fungi.
In its minor stages, this infection is asymptomatic. The majority of people learn about it during their dental check-ups. However, more severe cases can affect the quality of life and need more extensive treatment like surgery or laser therapy.
There are different reasons why this infection develops. Usually, it’s a result of poor hygiene, prolonged wearing, or some health condition. It is very common, but still, it is possible to prevent it. For that, you need to make sure that you’re maintaining good oral hygiene. In addition, it’s recommended that you get dental implants Turkey to prevent a poor fit from causing trauma to the tissue.
Lastly, you should get regular dental check-ups so that your dentist can assess whether your dentures are in good condition. If you’re experiencing any symptoms of denture stomatitis, you must reach out to your dentist immediately.
Reviewed and approved by Dr Izbel Aksit.